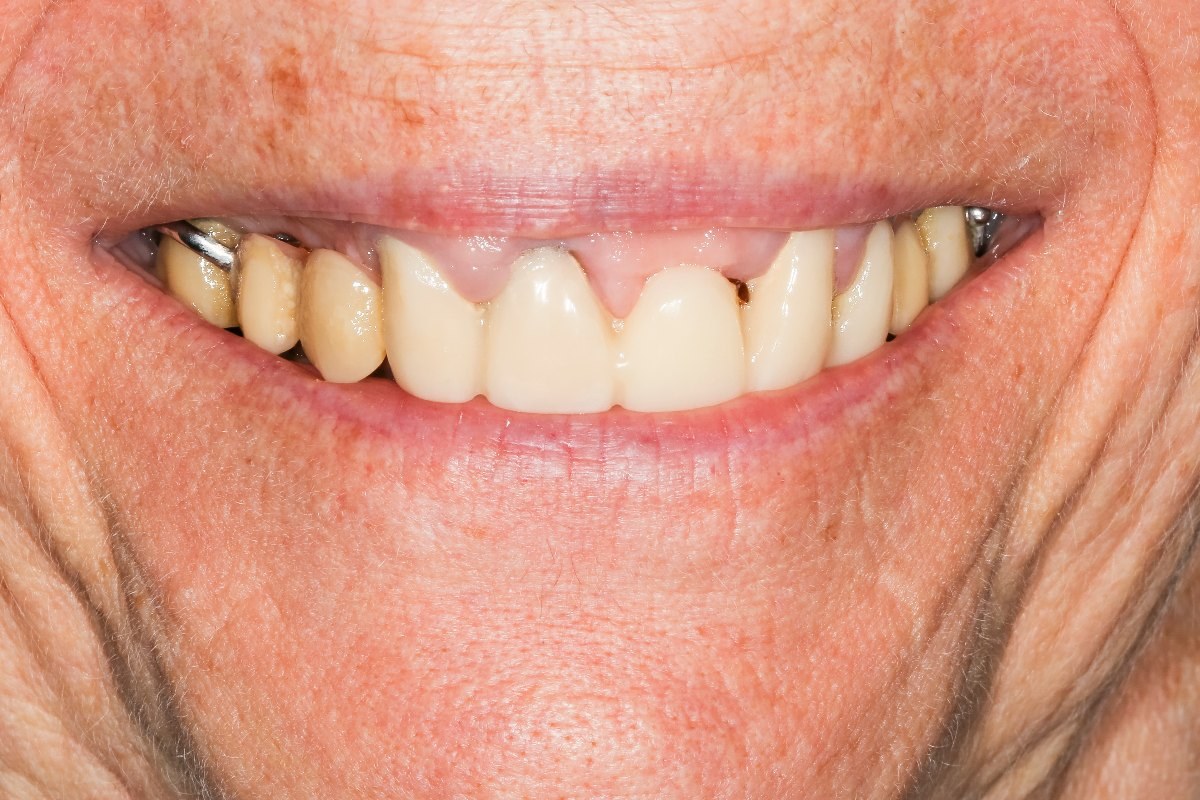
In dentistry, peri-implantitis is the term used to describe the advanced inflammation of the gums after implant placement. The implant-bed disease, which occurs in two stages, inevitably leads to the loss of the dental implant in its second stage if the patient's therapy is not timely. The sooner the treating dentist diagnoses peri-implantitis, the greater his chances of complete healing.
What is peri-implantitis?
Dental implants are a contemporary and aesthetically pleasing form of dentures that is becoming increasingly popular. They consist of a screw-like shaped dental implant neck made of tissue-friendly titanium, which is screwed into the jaws of the jaw and then fuses tightly with it. On the artificial tooth root the specialist for implantology fixes a structure with a ceramic crown. Only she is ultimately visible in the mouth. But as practical as modern dental implants are, they always harbor the risk of peri-implantitis.
How does a peri-implantitis develop?
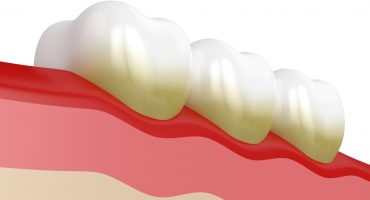
Implant bed inflammation, in its initial stage - they are called (peri-implant) mucositis - leads to inflammation of the gingival tissue directly in the vicinity of the implant. If you recognize them early and treat them accordingly, they heal completely.
However, if the patient suffers from peri-implantitis, the bacterial infection has progressed so much that the pathogens have already infected the jawbone. It forms untreated or too late, then returns in the following years, so that the implant loosens. The far advanced bone loss then requires a different kind of dentures.
Like periodontitis (tooth-bed inflammation), peri-implantitis is the result of bacterial infection. The dental implants, which are not sufficiently removed by the patient, ensure that the bacteria penetrate from the edge of the gum to the dental implant neck and cause the inflammation there.
Other causes of mucositis or peri-implantitis are:
- irregular dental checks
- insufficient or insufficiently treated periodontitis
- check defective implant healing
- certain general conditions such as diabetes mellitus and osteoporosis (calcium deficiency-related bone fragility)
- hormonal changes
- intake of immune-suppressing drugs (immunosuppressants)
- heavy smoking
- long-term stress
- a genetically induced increased risk of developing inflammation
Incidentally, peri-implantitis may also be caused in some cases by the treating dentist. It is therefore recommended that implants are only used by specialists in oral surgery and have them regularly checked there.
What are the symptoms of implant bed inflammation?
Initially, peri-implantitis manifests with a light touch pain that occurs whenever the patient touches the swollen gum near the implant. Sometimes the dentures themselves are painful. The gum line is reddish at the point in question. There is pus around the implant neck, which sometimes comes out by itself. If you are an implant wearer and you experience such symptoms, you should immediately consult a specialist in implantology.
In the further course of the disease, pain occurs in the area of the jawbone. It comes to the regression of the gums near the inserted artificial tooth root. The patient has the subjective feeling that his implant has relaxed. In addition, bad breath is noticeable. If bone loss is already well advanced, the dental implant will fall out. The bone substance can neither regenerate nor can it be rebuilt.
Diagnosis of peri-implantitis
The implantologist uses several methods to find out if the patient has peri-implantitis. With the aid of the completely pain-free marker test (aMMP-8-Tests), bone resorption in the oropharynx can be detected at an early stage. If the aMMP-8 collagenase value is increased in the patient, there is indeed a dental implant bed inflammation.
Collagenases are enzymes that specialize in the breakdown of tissue-substance. To perform the test, the examiner takes a sample near the implant using a test strip.
During the classic periodontal examination, the implantology specialist inserts the probe into the gingival pocket near the dental implant. If pus or blood escapes, inflammation of the implant bed is most likely present. Using an X-ray, he can determine exactly whether his suspected diagnosis is correct or not. He also sees on the radiograph, whether a structure of the jawbone (augmentation) makes sense.
Treatment Implantitis
In peri-implantitis therapy, complete elimination of inflammation is paramount. How the dentist does this determines the stage of the disease and the types of bacteria that predominate in the patient.
A mucositis - it merely infects the soft tissue immediately surrounding the implant - can be treated well with an antimicrobial rinse solution (chlorhexidine). Also, a photothermal therapy (PTT) using a special laser can be used to kill the pathogen responsible for tissue degradation. You disinfect the affected periodontal pockets. Therapeutic supplements include a professional tooth cleaning (PZR) and a professional cleaning of the dentures by the dentist. In addition, the patient often has to take additional antibiotics.
However, if the dentist diagnoses advanced peri-implantitis, he must surgically remove the artificial tooth root. If the bacterial inflammation then healed completely, he builds up the lost bone substance again. This requires further surgery. The implantologist fills the jawbone with bone substitute material. The bone thus has the opportunity to regenerate. Some time later, the physician can then insert another implant in the same place. An operative thickening of the gums around the dental implant is also a possible therapeutic option.
Prevention of Peri-Implantitis
In order to avoid the painful implant bed inflammation, implant specialists recommend that their patients
- regularly the control examinations
- professional implant cleaning
- undergo an x-ray examination per year in practice for implantology and
- regularly follow the after-care appointments.
Risk patients - ie persons with a hereditary increased risk of inflammation - should always have an aMMP-8 test performed at regular intervals.
Since the transition from the jawbone to the oral cavity is the critical site for implants, the implant wearer should drive a particularly thorough dental care. Because exactly at this point, the bacterial plaques are particularly happy to store. If they are not removed properly or not regularly, the pathogens migrate down the implant neck to the jawbone.
Implantologists recommend not brushing too hard with (electric) toothbrushes with a short head and the use of interdental brushes and dental floss. The interdental brushes are best used straight and only where the gaps are already larger.