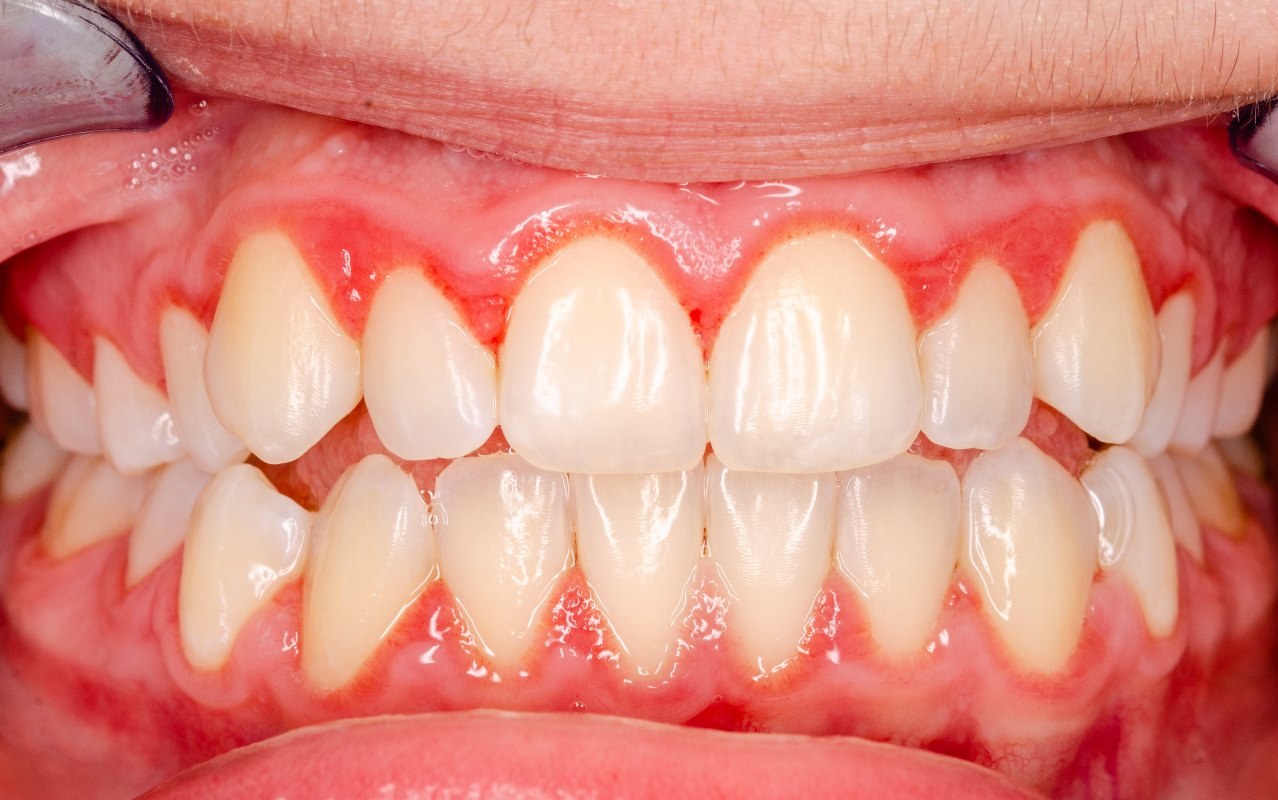
In dentistry, gingivitis is the acute or chronic inflammation of the gums. In acute inflammation, not the entire gum (gingiva) is affected, but only its upper part (gum line or margin).
What is a gingivitis?
In gingivitis, gingivitis is the name given to gingivitis acute or chronic. In acute inflammation, not the entire gum (gingiva), but only its upper part (gingival margin or hem) is affected.
An untreated or inadequately treated acute gingivitis is becoming chronic, which has far-reaching consequences for the entire dentition of the patient. In addition, it can cause inflammation of the oral mucosa (gingivostomatitis).
Gingivitis is caused by various types of pathogens (mixed infection) and is one of the most common infections of the oropharynx: Health experts assume that 4 out of 5 adults suffer from chronic or acute gingivitis.
To prevent the condition from even occurring, the patient should brush teeth thoroughly at least twice a day. It is also advisable to have a professional tooth cleaning performed once a year. It even cleans the areas that are hard to reach for toothbrushes.
Patients suffering from gingivitis should only use toothbrushes with soft, rounded bristles. They are also good for preventing gum disease if you tend to use more force when brushing your teeth.
Interdental toothbrushes and flossing help to remove food debris and plaque from the interdental spaces and thus also prevent gingivitis.
Causes of gingivitis
Gingivitis is mainly caused by abacterial mixed infection with various pathogens. However,are also the fungi and viruses trigger of the disease. The oral cavity, with more than 500 different bacterial species, is one of the regions of the human body that is colonized by most pathogens.
Inadequate oral hygiene due to infrequent or only superficial brushing of teeth ensures a rapid increase in the microbial oral flora. The bacteria release toxins, aggressive metabolic breakdown products and acids that can attack the gums. Under certain circumstances, it then comes to a gingivitis. Only a thorough cleaning of the teeth helps to eliminate the harmful bacterial plaques: not even the human immune system is so effective.
In addition, gingivitis can be caused by gum injuries. This can be done by the person scrubbing his teeth too hard: the pathogens and toxins contained in the plaque penetrate the gums and cause inflammation there. Also, gum irritation by certain dentifrice may be the cause of gum disease. Other causes are also diseases such as diabetes mellitus (diabetes) and certain metabolic diseases.
Other Possible triggers of gingivitis include:
- excessive alcohol consumption
- too much nicotine
- stress
- changes in hormone levels (puberty, pregnancy)
- vitamin C deficiency
- heavy metal poisoning
- certain medications (anti-epileptic drugs such as hydantoin, antihypertensive agents)
Whether it despite presence of bacterial dental plaque too In the end, the immune system decides gum infections occur. Patients with weakened immune system immune for those who immunosuppressants need to take (medicines that suppress pathological reactions of the system) are at an increased risk of developing gingivitis. The same applies to people who eat unhealthily, prefer to breathe through the mouth or have a low salivary flow.
Symptoms and course of gingivitis
In acute gingivitis, the patient has an inflamed, red and swollen gum line. He is softer than usual and prone to bleeding. In addition, the person has strong bad breath.
In Chronic gingivitis, the bacteria have already penetrated from the gingival margin to the jaw and damage there the entire periodontium. The gums have receded so that the necks and roots are exposed. The patient has severe pain and intense bad breath. The bacteria continue to multiply in the jaw, eventually causing the teeth to loosen and fail. In this case, dentistry speaks of periodontitis.
In rarer cases, even the gums between the teeth is infected. Then it is an acute necrotizing ulcerous gingivitis (ANUG). It causes the tissue of the interdental spaces to become ulcerated and eventually to decompose. The acute necrotizing form of gingivitis is manifested by the following symptoms:
- pain experiencing
- high-fever sudden onset
- drowsiness
- bad breath
Persons with such symptoms should seek dental treatment as soon as possible to prevent worsening gum disease.
How is a gingivitis diagnosed?
The gingivitis is already visible to the naked eye. The specialist in dentistry uses acheckspecial probe to the firmness of the gums and see if it has already formed gingival pockets. This refers to pocket-like enlarged gaps between the gingival margin and the tooth. This gap is not deeper than a maximum of 2 millimeters for healthy gums. In these gum pockets, the bacterial pathogens like to settle and fill the cavities with pus. Gum pockets are an indication that the patient is already suffering from periodontal disease.
If the gingivitis is already very advanced, even the careful touch of the gums with the probe triggers gum bleeding and pain: even the periodontium is affected by the inflammation. To check his suspected diagnosis, the dentist then makes an X-ray of the patient's jaw.
Saliva examination is used to determine the oral flora of the person affected. The laboratory analyzes all pathogens and marks the particularly aggressive germs on the test results sheet separately. This gives the dentist valuable information about which medications to administer for the treatment of gingivitis or periodontitis. In addition, the saliva test gives him information about whether his salivary flow rate contributed to the development of gingivitis or not.
How to treat gingivitis
First, with the help of a professional tooth cleaning, the dentist removes all dental plaque - even those that are in the interdental spaces. He removes the deposits in the periodontal pockets, drains the pathogens and pus and disinfects the cavity then thoroughly polishes the tooth surfaces. Then the dentist seals the teeth with fluoride varnish. So the pathogens can no longer commit to it.
The acute gingivitis patient can also treat himself in the first days. This often requires improved oral hygiene and some proven old home remedies. The patient may use the anti-inflammatory and anti-bacterial natural agents at home. These include, for example, teas from chamomile flowers or a glass of water with apple cider vinegar for mouthwash. However, if he still does not notice any improvement after a few days, he should seek the help of a dentist as soon as possible.
Weitere Beiträge

Caries (Tooth decay)
Tooth decay is the dental most common disease in industrialized countries. The term caries is derived from the Latin term caries and means putrefaction or rottenness. Dental caries (Caries dentium) is an infectious infection that can be transmitted from one person to another.